Our work with populations in Leeds goes beyond diagnosing and treating illness, putting more emphasis on improving well-being and preventing ill health.
Populations in Leeds
Our health and care needs are changing: our lifestyles are increasing our risk of preventable disease and are affecting our well-being. We are living longer with more multiple long-term conditions like asthma, diabetes, and heart disease – and avoidable and unfair differences in health between different groups of people is increasing (health inequality gap).
To address this, we need to move away from a system just focused on diagnosing and treating illness towards one that is based on promoting well-being and preventing ill health. We set out how we will do this in the Healthy Leeds Plan which underpins our population health approach.
Population health is a way of looking at health and care that aims to improve physical and mental health outcomes, promote well-being, and reduce health inequalities across the entire population, over the whole life course. This means we’re interested in building and maintaining the best long-term health possible for everyone. We know that this means more than just treating people when they get ill – it means building thriving communities where people are supported to live full, happy, healthy lives. We call this looking at the ‘wider determinants of health’, which includes things like the environment, jobs, school, deprivation, and culture. Follow this link for a great video explaining population health: https://www.kingsfund.org.uk/audio-video/population-health-animation
Of course, people have different needs, and what good health looks like varies between people. Someone living with a long-term disability might imagine the best health possible for them differently to a pregnant person or a child in school.
So, we look at the population of Leeds as a few defined groups of people who have similar health and care needs. We call these ‘segments’, and we have nine of them in Leeds–they’re the green boxes on the diagram below (there is a list below the image). By looking at our population in this way, we can better understand what people need to address the challenges they face, and how we as a health and care system can help.
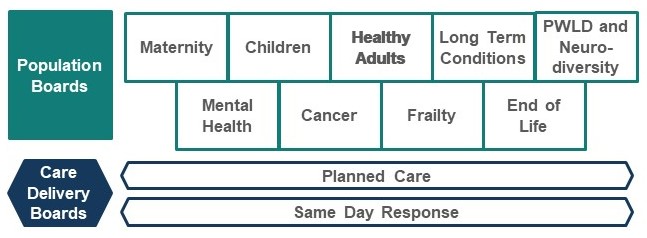
Population boards
In Leeds, each of these population segments has a group of senior staff – including doctors, public health experts, charities, the local council, and health system leaders – who are responsible for improving the population segment’s health and wellbeing. These groups are called ‘population boards’.
These boards will ensure that all key partners are involved in designing new ways of working which will improve health and well-being today as well as in future years’ time. The boards will work with local people and charities to make decisions about how we spend our budget in Leeds. By having everyone around the table, we can make sure our decisions are coordinated to improve every aspect of health and care.
Each population board will focus on its population as well as working with other boards to ensure resources are used in the way that best meets their needs. In this way, all the boards will work together to deliver the Healthy Leeds Plan.
Our population boards are:
- Cancer
- Children and young people
- End-of-life
- Frailty
- Healthy adults
- Learning disability and neurodiversity
- Long-term conditions
- Maternity
- Mental health
Care delivery boards
We also have two other boards, called ‘care delivery boards’. These have the same senior membership and responsibilities as the population boards above, but instead of having a population they are responsible for, the board instead looks at specific services to improve how we work with all populations.
Primary care board
We also have a primary care board. This board has the same senior membership and responsibilities as the population boards above, but instead of having a population they are responsible for, the board instead looks at specific services to improve how we work with all populations.
Find out more
You can find out more about our population boards here by following the links below. We are currently working on setting up pages for each of the boards.
You can find out more about population health on the NHS England website here: https://www.england.nhs.uk/integratedcare/what-is-integrated-care/phm/
Population boards
Cancer
People who have been diagnosed with cancer, or had cancer treatment, within the last five years.
Find out more about the cancer population board
Children and young people
Everyone who is under the age of 18, except for pregnant people whose care is covered by the maternity board.
Find out more about the children and young people's population board
End of Life
People who are approaching the end of their life, meaning they are expected to be within the last year of life.
Find out more about the end-of-life population board
Frailty
People who are living with frailty, and therefore struggle with many aspects of day-to-day life. This is usually to do with age, with most people in this group over the age of 65 and living with a number of long-term conditions. This group also includes people living with dementia.
Find out more about the frailty population board
Healthy Adults
Adults who are generally healthy, meaning that they don’t have any diagnosed long-term conditions, and aren’t pregnant. This doesn’t necessarily mean they feel healthy all the time, just that they are not currently diagnosed with a long-term condition.
Find out more about the healthy adults population board
Learning disability and neurodiversity
People whose brain processes, learns, and / or behaves differently from what is considered “typical” such as autistic people. This does not include more mild learning difficulties such as dyslexia.
Find out more about the learning disability and neurodiversity population board
Long-term conditions
People with long-term conditions such as diabetes, asthma, or cardiovascular disease.
Find out more about the long-term conditions population board
Maternity
People who are currently pregnant, or are within two years of giving birth.
Find out more about the maternity population board
Mental health
People who are living with severe mental illness, such as schizophrenia. This board also works with the other boards around supporting people in their populations with more common mental illnesses, such as depression or anxiety.
Find out more about the mental health population board
Care delivery boards
Planned care
Services that offer planned appointments or interventions, such as joint replacements and cataract surgery.
Find out more about the planned care delivery board
Primary care
Primary care services provide the first point of contact in the healthcare system, acting as the ‘front door’ of the NHS. Primary care includes general practice, community pharmacy, dental, and optometry (eye health) services.’
Find out more about the primary care board
Same-day emergency response
Services that provide care urgently or in an emergency, on the same day. This includes, among other things, the emergency department (accident and emergency), same-day primary care, and 111.
Find out more about the same-day response care delivery board
Public involvement workshops
We will be holding public involvement workshops to check the findings of our insight reports, review our identified outcomes for each board, and discuss our approach to public involvement on the boards.
The workshops are open to anyone with an interest in the focus of each board. They will be held virtually on Zoom.
Don’t worry if you can’t attend the dates of the workshops, there will be other ways to get involved in each of the boards and share your feedback. We are also recording each workshop so you can watch the workshop when you are able.
Follow the links below to find out how to book on to the workshop:
Upcoming workshops
- Cancer – Thursday 30 March 2023, 10am -12pm
- Children and young people – Tuesday 7 March 2023, 2pm – 4pm
- Healthy adults – Wednesday 5 April 2023, 1pm – 3pm
- Learning disability and neurodiversity – Monday 13 March 2023, 1pm – 4pm
- Same-day response – original date postponed, new date to be confirmed soon
Completed workshops
- End-of-life – 10 November 2022, 1pm – 3pm (recording of workshop available via link)
- Frailty – Wednesday 11 January 2023, 2:30pm – 4:30pm (recording of workshop available via link soon)
- Long-term conditions – Wednesday 1 February 2023, 9am – 11am (recording of workshop available via link soon)
- Maternity – Wednesday 25 January 2023, 9am – 11am (recording of workshop available via link soon)
- Mental health – Monday 20 February 2023, 2pm – 4pm (recording of workshop available via link soon)
- Planned care – Wednesday 1 March 2023, 1pm – 3pm (recording of workshop available via link soon)
- Primary care – Tuesday 28 February 2023, 5pm – 7pm (recording of workshop available via link soon)